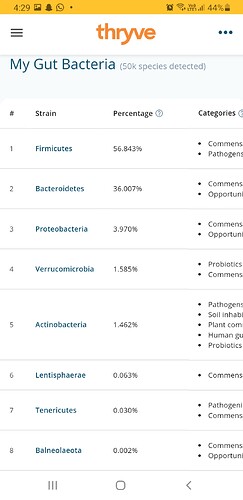
Still looking at this. Some notes.
Microbiome–host systems interactions: protective effects of propionate upon the blood–brain barrier
Gut microbiota composition and function are symbiotically linked with host health and altered in metabolic, inflammatory and neurodegenerative disorders. Three recognised mechanisms exist by which the microbiome influences the gut–brain axis: modification of autonomic/sensorimotor connections, immune activation, and neuroendocrine pathway regulation. We hypothesised interactions between circulating gut-derived microbial metabolites, and the blood–brain barrier (BBB) also contribute to the gut–brain axis. Propionate, produced from dietary substrates by colonic bacteria, stimulates intestinal gluconeogenesis and is associated with reduced stress behaviours, but its potential endocrine role has not been addressed.
After demonstrating expression of the propionate receptor FFAR3 on human brain endothelium, we examined the impact of a physiologically relevant propionate concentration (1 μM) on BBB properties in vitro. Propionate inhibited pathways associated with non-specific microbial infections via a CD14-dependent mechanism, suppressed expression of LRP-1 and protected the BBB from oxidative stress via NRF2 (NFE2L2) signalling.
The gut microbiome harbours 150 times more genes than the human genome, significantly increasing the repertoire of functional genes available to the host and contributing to the harvesting of energy from food
It is clear, however, that gut-derived microbial metabolites and products such as lipopolysaccharide (LPS) can influence human health both in the intestine and systemically [12, 13], with reported effects ranging from mediation of xenobiotic toxicity [14], through modification of the risk of preterm birth [15] to induction of epigenetic programming in multiple host tissues [16,
gut microbe-depleted animals have been shown to exhibit changes in serotonergic and glutamatergic neuronal signalling [20] and expression of brain-derived neurotrophic factor (BDNF) within the limbic system [22, 23], providing a molecular correlate for behavioural changes.
data highlight a potential role for short-chain fatty acids (SCFAs) as key microbial mediators in the gut–brain axis
The majority of studies looking at the role of SCFAs in the gut–brain axis have focused on butyrate [40], with relatively few investigating propionate despite its similar plasma concentration and receptor affinity. Propionate is a highly potent FFAR3 agonist for its size (agonist activity GTPγS pEC50 ( E max) 3.9–5.7(100%)) and is close to optimal ligand efficiency (−Δ G = 1.26 kcal mol−1 atom−1) for this receptor [41]. While propionate has been shown to stimulate intestinal gluconeogenesis through direct stimulation of enteric–CNS pathways [42] and increased intestinal propionate has been associated with reduced stress behaviours [43] and reward pathway activity
Given the critical gate-keeping role the BBB plays in communication between the periphery and the brain parenchyma, our findings set the stage for future investigation of the influence the gut microbiota has on this structure and the impact intestinal dysbiosis may have upon individual susceptibility to neurological and psychological diseases.
Our findings thus cement SCFAs as a key group of gut-derived microbial mediators modulating BBB function and provide evidence emphasising a direct action through the circulation.

 . That said, I still needed little AI + Proviron to balance T:E2. On the other hand, Testosterone enanthate was far more subtle in its effect, sort of slow acting.
. That said, I still needed little AI + Proviron to balance T:E2. On the other hand, Testosterone enanthate was far more subtle in its effect, sort of slow acting. need to kick excessive inflammation outta my life!
need to kick excessive inflammation outta my life!